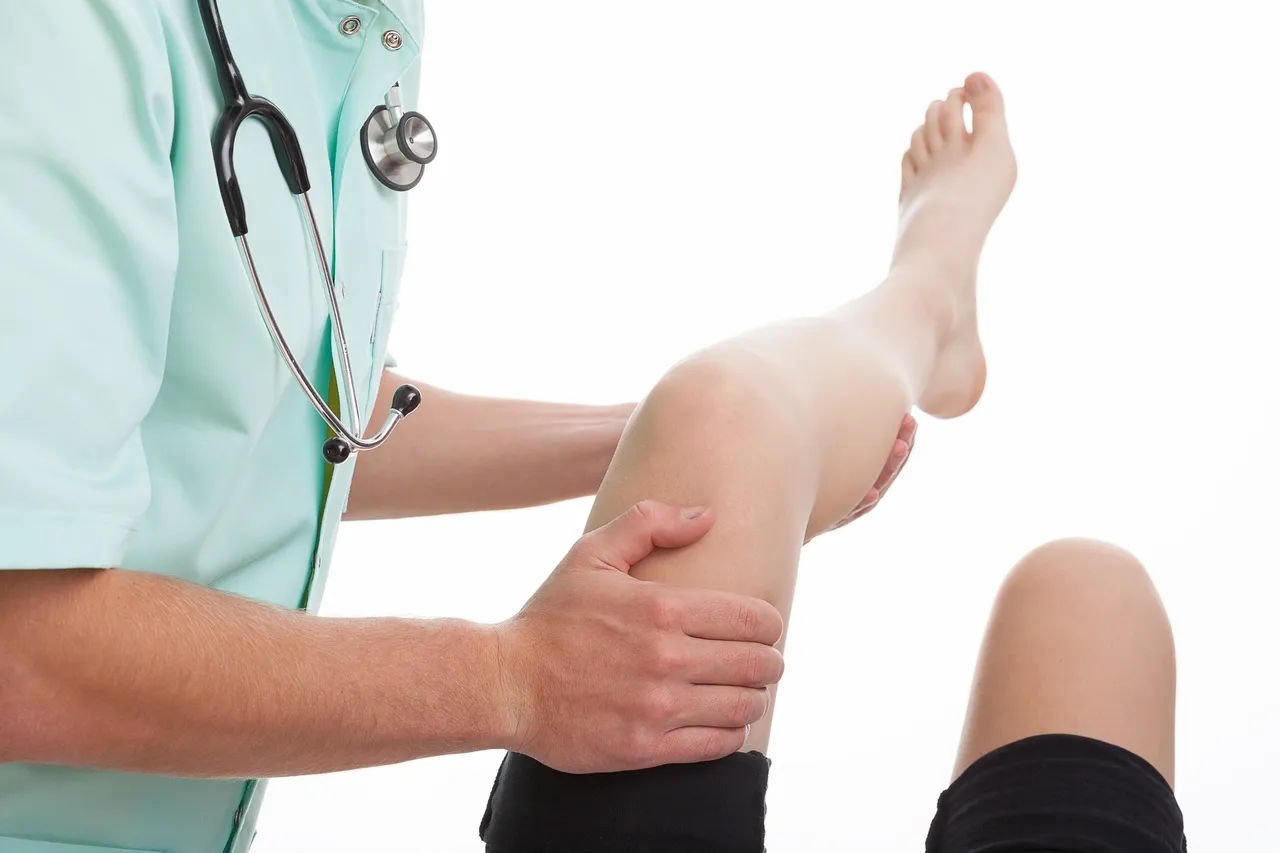
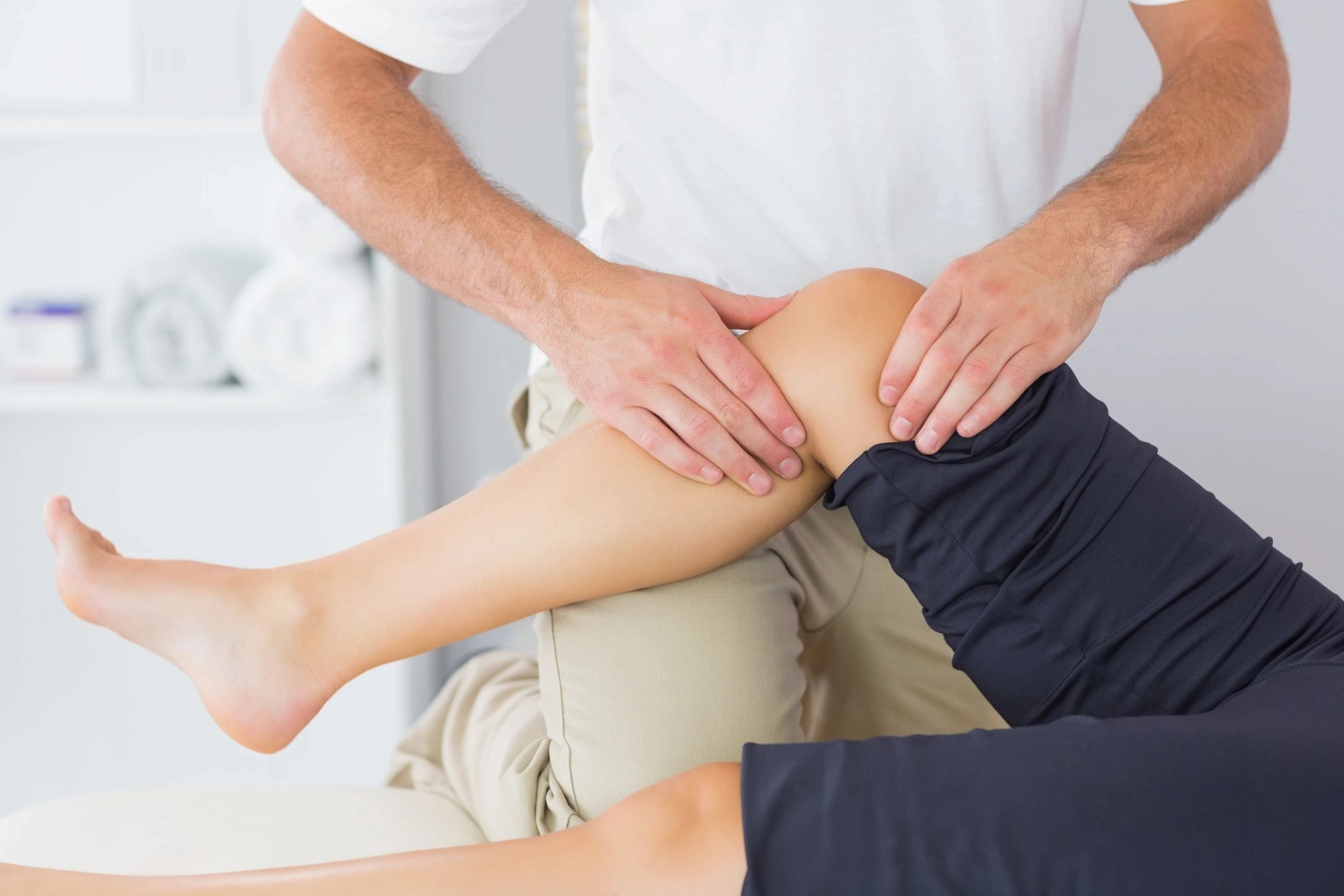
Knee pain is very common but also very treatable. Today’s post will be going over the various things that may be contributing to your knee pain and what can be done about them. This will include ideas you can use for yourself, but always keep in mind that consulting a specialist like a physical therapist will make the process much easier.
Referred pain
We’ll start with pain that is felt in the knee, but may be caused by something else. It’s possible for the hip or the low back to refer pain to the knee. Pain that comes from the hip will usually hurt worse going up stairs than going down stairs. Pain that is truly from the knee almost always hurts worse going down stairs. Another hip sign can be found when you lie on your back with your knee bent and then let it fall out to the side to open your hip up. If this increases your pain, it’s likely that the hip is contributing because this motion doesn’t use knee motion, it just changes the hip position. Finally, signs of significant hip weakness might implicate the hip. The most noticeable sign is called ‘hip drop’ or a Trendelenburg gait. If when you’re walking, one side of your hips drops down with every step, it’s an indication that the hip you’re standing on is weak. If you suspect your hip is contributing to your pain, you can start strengthening the hip by doing side lying leg raises, using a cane if you have hip drop, and, as always, consulting a physical therapist.
Knee pain can also come from the low back. While this will often be pain that radiates from the back or hip itself all the way down to the knee, sometimes it can just be felt only at the knee. If your back is contributing, then in general, trunk motions will increase your pain. You can test this by first sitting down to take your legs out of the consideration. Then test moving your back in all directions. You’ll move into each direction 10 times in a controlled fashion. Start by bending forward 10 times. Then lean backwards. Next, bend to each side. Finally, try rotating left and right each.
If any of these motions cause knee pain, then it will be best to consult a rehabilitation expert. They will likely help you improve your trunk strength with exercises, improve your flexibility with some stretches, teach you to move in ways that puts less stress on your back, and use manual therapy on your back.
Movement patterns
Now onto things that directly overload the knee itself. There are 3 movement patterns, often with specific muscle imbalances in both strength and flexibility, that can contribute to overloading the knee.
Knee bending pattern: this is when someone often uses their knees to move their body more than necessary. If you were to pick something up from the ground, you could use your knees, hips, and back to different amounts. The more you squat down, the more your load your knees. The more you bend over, the more you use your hips and back. While one strategy isn’t necessary better than the others, if a segment is hurting, then it makes sense to shift away from using that part. So if your knees hurt, then using your hips more will shift load away from the knees – this will involve folding your trunk over more at the hips. This pattern of using the hips more can be generalized to many activities which include standing up from a chair, going up/down stairs, picking things up, walking on level ground and slants, and getting in/out of the car.
The more you use your knees, the more upright your trunk will be and the more your knees will go forward over your toes. The more you use your hips, the more your trunk will fold over and your shins will stay vertical. So if you want to practice using your hips more, you can think about folding over more and not letting your knees go forward over your toes.
Knee going inward pattern: many people’s knees will move inward towards the middle of their body whenever they use their legs to push such as going up/down stairs or standing from a chair. This is especially true of women due to them usually having wider hips. The knee will go inward as will as rotate inward. Since it can put the knee cap in a less efficient position, the increased pressure on the front of the knee can lead to pain (patellofemoral pain syndrome). The rotation of the knee inward can cause twisting at the knee which can lead to pain on the sides of the knee as well. Controlling the knee position is actually the responsibility of the hip muscles so exercises to strengthen the outside of the hip are key. Start with side leg lifts and clamshells and move up to standing exercises. An advanced exercise often used is walking sideways with a band around the legs.
For people who don’t do sports, being able to rise from a chair and go up/down stairs with good knee alignment is often sufficient to address this problem. For very active people, they will want to be able to keep their knees in good alignment with advanced activities including landing from a jump and single leg hopping.
Knee going backwards pattern: if you ever had an event where you hyperextended your knee – it went backwards too far – then you may have pain in the back of your knee. Sometimes this keeps happening because of laxity in the ligaments of the knee. Practicing normal movement patterns is more important in this case than exercises for strength usually. The goal is to learn to straighten the knee a normal amount. If you’re seeing a physical therapist, they can help provide feedback. If you’re practicing on your own, you’ll need a mirror from the side to see your knee position. I’ll often educate people on the ‘soft knee’ position – avoiding completely locking your knees. You’ll want to start by lying down and slowing straightening the knee while watching your knee position in the mirror. Focus on learning what it feels like when you’re in the proper straight position. Then work on this in other patterns such as standing, then standing up from a chair, going up stairs, all the way to squatting (if you lift weights) and jumping.
The other possibility with repeated hyperextension is if your ankle can’t flex. When the ankle can’t flex forward, the rest of the leg has to do something in order to get your center of gravity forward to walk. There are a couple of things your body can do to awkwardly make this work, and one of them is to slightly hyperextend the knee. If this is your problem, you will know it because you have ankle problems. This isn’t something that happens without very significant ankle flexibility limitations. The true solution is to increase your ankle flexibility. If you’re dealing with significant limitations in your ankle, it is best to consult a physical therapist for specific treatment. This will generally involve a variety of different stretches as well as manual therapy to help loosen up restrictions in the joint and soft tissues.
Nervous system
When you’ve had pain for longer than 6 months, your nervous system will have made several changes that makes your body more sensitive to pain signals. This happens at the nerves of the knee, the spine, and all the way up to the knee ‘area’ of the brain itself. One of the best ways to desensitize the nervous system is education. Many people believe that exercise might be bad for the knee or their pain will never go away. Research shows that exercise is actually very helpful for the knee, especially in cases of arthritis. Just understanding that things like exercise and massage can help lessen or even eliminate the pain can change the way your nervous system monitors sensitivity in the knee.
There are more specific techniques as well that often include guided visualization or imagery. Since this almost exclusively is directed at the brain and nervous system, it is effective at ‘re-programming’ the ‘software‘ of the body. You can imagine whatever helpful imagery makes sense to you, whether that is walking around in a healing pool of water or imaging bathing your leg in warm sunlight at the beach to anything else. If you don’t know how to do any of this, consult a hypnotist who uses in guided visualization.
Nerves of the knee
There are 2 main nerves that supply the knee: the femoral nerve (front and medial sides) and the sciatic nerve (back and lateral [outside] sides). These often contribute to pain so getting the nerves back to normal is helpful.
Sciatic nerve: test this by going into a hamstring stretch. Once you can feel a light stretch, roll your chin down to your chest. It’s normal to feel an increase in the stretch in the back of your calf and your thigh. But, if doing this causes knee pain, then you may have nerve tension. Below is an easy to follow video you can use to start working it out.
Femoral nerve: test this by going into a quad stretch. Lie on your side with the leg you’re testing on top. Wrap a belt or strap around your ankle and then gently pull the strap to bend your knee. Keep the hip straight so that the thigh stays on top of the bottom leg. This will be a quad stretch. Once you feel a light stretch, roll your chin to your chest like you’re curling into a ball. If this causes knee pain, you may have femoral nerve tension. Below is a video on an exercise to start mobilizing or ‘flossing’ the nerve.
Manual therapy
Often, tender points in the soft tissues of the leg can contribute to or even cause knee pain. The skin, muscles, tendons, ligaments, and/or scar tissue can all contribute. You can feel on your own leg for these tender spots and then gently work on them using your hands or soft tissue instruments. Even though these spots may feel like knots, they are not physical lumps you can just mash away. Often they are contracted muscles, adhesions in the fascia, small points of fluid build-up, or even just normal structures like the surfaces of the bones or ligaments in your leg. If you press on them for a few seconds and they refer pain to your knee, then they are probably more important. If you press on them and they don’t, it’s likely they aren’t important. When treating them, use gentle pressure and massage – more pressure is not any more effective and is much more likely to make you sore afterwards.
As you go through this process, you can treat tender points as you notice them. Or you can note them and how tender they are then keep going. Once you’re completely done, you would start by treating the most tender points first. Often after you’ve treated the most tender ones, other ones will have gone away or become less tender.
Start at the front of your hip and work your way straight down to the knee cap. Then start back up at the hip, go an inch or so to the side and work back down. Repeat on both sides until you’ve covered the front of your thigh from the hip to the knee cap. Then relax your leg and gently move your knee cap side to side. It should move freely.
Now the inside of your leg. Start at the very top inside part of your knee which will be at the groin muscles. Do the same procedure as before: start at the top and work all the way down to the knee. Then start over and a little to the side and keep working until you cover the inside of your thigh.
Do the same process for the outside of your leg. Start at the top of your hip, under the crest of your pelvis. Make sure you feel through your butt muscles in your hip as well.
Finally, repeat for the back of your thigh. Cover the entire back of your leg to the back of your knee.